|
Exercise For Back Pain
Author:
Stan Reents, PharmD
Original Posting:
05/06/2007 06:56 AM
Last Revision: 09/15/2020 10:35 AM
 Back pain affects 60-80% of American adults at some time during their lives, and it is estimated that up to 50% have back pain within any given year. Back pain symptoms are among the top 10 reasons for visits to emergency rooms and physicians' offices. Back pain is the most common disability for persons under age 45. Back pain affects 60-80% of American adults at some time during their lives, and it is estimated that up to 50% have back pain within any given year. Back pain symptoms are among the top 10 reasons for visits to emergency rooms and physicians' offices. Back pain is the most common disability for persons under age 45.
ACUTE vs. CHRONIC BACK PAIN The condition is diagnosed as acute if lasting less than a month and not caused by serious medical conditions. Most cases clear up in a few days, although recurrence after a first attack is common. Low back symptoms are usually acute and self-limited. However, pain often recurs, and in 5-10% of patients, back pain becomes chronic. Low back pain is considered chronic when it persists beyond 3 months (Mannion AF, et al. 2001). Adolescents can experience back pain, too, but usually for different reasons than adults (see below). CAUSES OF BACK PAIN While some back injuries are related to lifting and various repetitive motion activities, in more than 80% of back pain cases, the cause is often unknown (Hadler NM, et al. 2007). Some of the known causes of back pain include: - Posture-related causes: poor posture while sitting or standing, discrepancies in leg length leading to an uneven pelvis, etc.
- Disordered spine anatomy: bone spurs on the vertebrae, spinal stenosis, herniated disc
- Obesity: a large belly, combined with weak abdominal muscles, pulls the spinal column forward and out of alignment
- Systemic diseases: osteoporosis, cancer, infection, osteoarthritis
ANATOMY OF THE SPINE The spine is a column of small bones called vertebrae that support the entire upper body. The column is grouped into sections, listed here from top to bottom:
AREA
OF THE SPINE | NUMBER OF
VERTEBRAE | DESCRIPTION | | • Cervical | 7 vertebrae | supports the neck | | • Thoracic | 12 vertebrae | supports the rib cage | | • Lumbar | 5 vertebrae | makes up the low back | | • Sacrum | 1 vertebrae | a shield-shaped bony structure
that connects with the pelvis | | • Coccyx | 4 vertebrae | the tail bone |
These vertebrae are each separated by small cartilaginous cushions known as intervertebral discs. Each vertebra surrounds and protects an arch-shaped central opening, which encloses the spinal cord. Nerves pass from the spinal cord to other parts of the body through small openings between each vertebra. Because the lumbar area of the spine supports most of the body's weight and stress, it is a common location for back pain. LACK OF EXERCISE AS A CAUSE OF BACK PAIN A 2011 survey by the CDC revealed that only 52% of adults in the US met the minimum recommendations for aerobic exercise and only 29% met the minimum recommendations for resistance exercise (Harris CD, et al. 2013). It turns out that lack of regular exercise is one of the most common causes of back pain. Lower back pain is very common in western, industrialized countries (Volinn E. 1997). And, rates of exercise are also very low in these countries. Is this purely coincidence? Unlikely. In one study, only 47% of persons suffering from low-back pain exercised regularly, whereas 86% of people without back pain exercised regularly (Cox JM, et al. 1987). A study from Denmark revealed that middle-age people who exercise for at least 3 hrs per week have a reduced risk of low-back pain (Harreby M, et al. 1997). TOO MUCH EXERCISE CAN CAUSE BACK PAIN, TOO Some activities, or, too much exercise, can actually be the cause of back pain. As sporting events become more aggressive and the activities become more specialized, particular types of back pain tend to increase. In adolescents, the number one cause of back pain is a condition called spondylolysis. It can develop in young athletes, between the ages of 10 and 15 years old, who are involved in sports that require repetitive hyperextension of the lower back as occurs when leaning backwards during gymnastics. Even low-impact sports such as swimming and tennis can cause back pain (Nyska M, et al. 2000). Elite athletes can develop back pain, too. At the 2000 Summer Olympics in Sydney, athletes with back pain were found to have a higher prevalence and a greater degree of lumbar disc degeneration than the normal population (Ong A, et al. 2003). Fortunately, most sports do not appear to increase the risk of herniated discs (Mundt DJ, et al. 1993), something that is fairly common in sedentary people. EXERCISE AS THERAPY FOR BACK PAIN As mentioned above, people who exercise regularly have lower rates of back pain (Cox JM, et al. 1987). The American Academy of Family Physicians recommends "back-conditioning exercises" for persons aged 19-64 years who are at increased risk for low back injury because of past history, obesity, or inactivity. But, is there any proof that exercise is better than other therapies for people who suffer from simple back pain? Yes! Exercise has been compared to other common treatments for back pain: Exercise vs. Spinal Manipulation: Considering how often it is performed, evidence supporting the benefit of spinal manipulation for simple low back pain is surprisingly limited. Several groups of experts reviewed the published literature to compare which is better: exercise vs. spinal manipulation: • The Cochrane Review Group evaluated the effectiveness of spinal manipulation for both acute low back pain and chronic low back pain against 7 other types of medical treatment, one of which was exercise. They found that spinal manipulation was no better than these other therapies. However, they included research that had a follow-up period of as short as 1 day (Assendelft WJ, et al. 2003). • Several years later, a separate group performed another literature review, evaluating exercise vs. spinal manipulation. Their criteria were much more strict, and, thus, only 2 published studies were evaluated. They found that one study endorsed exercise and the other one favored spinal manipulation. The authors concluded that both can be effective, but, if no improvement is seen within 8 weeks, then another treatment strategy should be pursued (Standaert CJ, et al. 2011). Exercise vs. Stretching + Traction: In a small Swedish study, patients who had had low back pain for 6 weeks or longer were treated with strength-training exercise of the abdominal and lumbar areas, or with manual therapy (stretching, traction). Assessments at 3 months and 12 months showed that the patients who participated in strength-training improved more than the manual therapy group. In addition, the strength-training group required less treatment for recurrent back pain than the manual therapy group (Rassmussen-Barr E, et al. 2003). EXERCISE PRINCIPLES Exercising the back is not as simple as lifting more and more weight to increase the strength of your back muscles. In addition, there are many different types of exercise: they should not considered equally effective. Stuart M. McGill, PhD, a professor at the University of Waterloo in Ontario, Canada, is a recognized expert in spine injuries and rehabilitation. He has published extensively on spine management. Surprisingly, McGill claims that stretching and muscular strength are not as critical to low back health as you might expect (McGill SM. 2001) (McGill S. 2010): • Flexibility: It is commonly thought that stretching the back and increasing its range of motion is beneficial and reduces back problems. However, according to Dr. McGill, people with a greater range of motion in their back (ie., think of gymnasts who can easily do back-bends) have an increased risk of future trouble (McGill S. 2010). Thus, this casts doubt on the benefits of excessive stretching to relieve back problems. Dr. McGill specifically warns against bending at the waist to touch your toes (ie., "spine flexion") first thing when you get out of bed (McGill S. 2010). • Muscular Strength: Here again, according to McGill, misconceptions arise. While it seems logical to conclude that back pain is a result of weak back muscles, in fact, improving the strength of the back muscles has little association with low-back health (McGill S. 2010). Indeed, some people injure their back in the process of trying to increase the strength of their back muscles because they perform the wrong type of exercise and work against too much resistance. • Muscular Endurance: McGill recommends that resistance-training programs for the back be designed to increase muscular endurance, as opposed to muscular strength (McGill S. 2010). When using weights to achieve this, the weight should be kept low and the number of repetitions should be relatively high. For example, in a Norwegian study, subjects with chronic low back pain performed 7-9 different exercises, either with free weights or weight-machines. For each exercise, 2-3 sets of 20-30 repetitions per set! were performed (Tortenson TA, et al. 1998). This works out to 40-90 reps per exercise, or, nearly 800 total reps per exercise session! So, the 2 key principles to consider when using exercise for non-serious back pain are: • increase muscular endurance, not muscular strength • "toning-up" the core muscles that surround and support the spine is more important than increasing flexibility in the spine RECOMMENDED EXERCISES FOR THE BACK Dr. McGill recommends these 3 exercises for most people with simple low-back pain (McGill S. 2010):
| FOR THESE MUSCLES: | DO THIS EXERCISE: | | • Abs | modified crunches | | • Sides | side bridge | | • Low-back | bird-dog |
Modified Crunches: Lie on your back, with your hands, a pillow, or a rolled-up towel under your lower back. One leg should be straight, flat against the floor. The other leg should be bent with your foot flat on the floor. (Your legs should be together, one straight, one bent.) Now, contract your abdominal muscles to lift your head and shoulders off the ground slightly, but do not do a complete sit-up. You should be looking at the ceiling during the contraction, not towards your feet. Do 10, then reverse the positioning of your legs and do another 10. • AVOID THIS: When doing modified crunches, do not flatten your lower back against the floor. The spine is not perfectly straight. So, flattening the low back violates the "spine neutral" position that should be maintained when doing crunches. You also do not need to do a full sit-up or crunch. Just contract your stomach muscles enough to lift your head and shoulders off the ground. Side Bridge: This is an isometric exercise for the muscles on the sides of your torso (abdominal obliques, quadratus lumborum). Start by lying on your side. Raise your body off the floor by resting on the elbow of your lower arm. (Keep your hand and forearm also on the floor for added stability.) Keep your body (and spine) straight, so that your hips are also off of the floor. At this point, only your forearm and the sides of your feet should be touching the floor. If this is too difficult, then bend your knees and support your body with your knees instead of your feet. • AVOID THIS: Do not hold these positions for longer than 8-10 seconds. Birddog: This exercise is a yoga-like isometric. Start with your hands and knees on the floor. Extend 1 leg straight out behind you, keeping it level with the ground. Extend your arm on the opposite side straight out in front of you, also keeping it level with the ground. Your head should be positioned so that you are looking down at the floor. • AVOID THIS: Do not hold these positions for longer than 8-10 seconds. Research shows that sustained contraction of the torso muscles causes them to lose oxygen rapidly (McGill SM, et al. 2000). Instead, build up your muscular endurance by doing more reps, NOT by holding each position as long as you can. The exercises described above should be done 5-7 days per week. In the past, Dr. McGill has also recommended this simple exercise: Cat-Camel: Start by getting on the floor on your hands and knees. Make sure your knees are at a 90-degree angle and your hips are directly above your knees. Tip your head down while raising your back upwards (keep your hands on the floor). At this point, the line from your head to your hips should resemble a continuous curve. Next, raise your head up so that you are looking forward while letting your belly hang down. Your lower back and your thighs should be forming a 90-degree angle (your hips should still be directly above your knees). Keep in mind that this is a "motion" exercise; ie., it is not a stretch. So, alternate back and forth between these 2 positions in a fluid movement. Do 5-8 cycles of this exercise. • AVOID THIS: When doing the cat-camel exercise, do not hold your body motionless in either position. STABILITY BALL EXERCISES 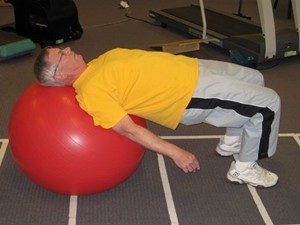 Stability balls are those colorful, plastic balls that are big enough to sit on. It turns out that doing exercises while sitting or lying on a stability ball is a good way to train the variety of muscles in your core. Stability ball exercises are also effective for people with simple low back pain. In these 2 photos, Bill is demonstrating several of these exercises: In the lying position, he places his head, neck, and shoulders on the ball, with both feet flat on the floor, then raises and lowers his hips. After you have lifted your hips up, Dr. McGill recommends holding this position in an isometric contraction for several seconds, then, relax. Repeat for a total of 10 contractions (McGill S. 2010). Another option in this same lying position is to roll your spine back and forth across the top of the ball. This will not only develop your core muscles, but will also provide a nice stretch.  In the seated position, the goal is to slowly and carefully rotate your upper torso (eg., shoulders) from one side to the other. Extending your arms out in front of you helps to keep your spine vertical as you move through the entire range of motion. However, Dr. McGill does not endorse exercises that twist the spine, even this one which doesn't actually restrict the hips from moving (McGill S. 2010). OTHER "BACK-FRIENDLY" ACTIVITIES • Aquatic Exercise: Aquatic exercise has been used to treat chronic low back pain. A study from Turkey showed that 5 sessions per week for 4 weeks was superior to non-aquatic home-based exercise (Dundar U, et al. 2009). However, a review of all published research on aquatic exercise, conducted in 2009, revealed only 7 acceptable studies. The conclusion from this literature review was that, while aquatic exercise was beneficial, it was no better than other strategies (Waller B, et al. 2009). • Aerobics: Researchers from Switzerland demonstrated that a combination of aerobics classes with stretching was just as effective as strengthening exercises using weight machines for adults with chronic low back pain. In this study, aerobics sessions were held twice per week for 3 months (total = 24 sessions). Each session lasted 1 hour and consisted of stretching, aerobic exercises, and muscle-toning exercises. The first 15 minutes involved whole-body static stretching and low-impact aerobic exercise, followed by 30 minutes of exercises targeting the trunk and leg muscles. The final 15 minutes of each session consisted of cool-down and relaxation exercises (Mannion AF, et al. 1999) (Mannion AF, et al. 2001). • Pilates: Pilates is an excellent method to develop "core" strength (eg., the muscles of the torso). But can it be helpful for patients with back pain? Yes. An Australian group compared 8 weeks of "trunk exercises" (Pilates) to stationary cycling in patients with chronic non-specific low back pain. They found that, at the end of the study, disability and pain improved more in the group that received Pilates exercise. However, 6 months after the study ended, symptoms were no different in the 2 groups (Marshall PW, et al. 2013). In another study, 1-hr of Pilates exercise 3 times a week for 12 weeks, was effective for patients with ankylosing spondylitis. Improvement was noted at the end of the study (ie., after 12-weeks of exercise) and 12 weeks later (Altan L, et al. 2012). • Swimming: Because it combines low resistance with high repetitions, swimming would seem to be an ideal activity for people with back pain. We are not aware of any research studies evaluating the benefit of swimming on back pain, however, one study showed that "aquatic exercise", which included walking in water and swimming, was beneficial for back pain if performed at least twice per week (Ariyoshi M, et al. 1999). • Walking: In one study, walking was less effective than physiotherapy and weight-training therapies for back pain: Subjects were asked to walk 1 hour per day, 3 times per week, for 12 weeks. Patients were allowed to walk on their own, so how far or how fast they walked was not determined (Tortenson TA, et al. 1998). • Yoga: In people who do not currently have back pain, yoga can be beneficial. Like Pilates, yoga is a good way to develop core strength. However, because some of the positions hyperextend, and/or put strain on the lower back, avoid yoga until after you have been pain-free for 6 months. Whatever you choose, select low-impact activities, and avoid those that demand high-risk moves. Sports that involve a lot of twisting (golf, tennis), quick stops and starts (basketball, racquetball) and contact sports (football, rugby) pose the greatest risks to your back. Also be cautious of activities that force you to hold your posture in an uncomfortable position, for example, riding a racing bike and in-line skating where you are bent over, or water-skiing and wind-surfing which require you to contract your back muscles for sustained periods of time. EXERCISES TO AVOID • Spine-twisting exercises: NEVER use exercise machines where half of your spine is anchored in place motionless while the other half of your spine rotates. • Straight Leg-Lifts: Leg-lifts put a tremendous amount of strain on your lower back. To lift your legs off the ground while lying on your back, the hip flexors pull against the pelvis, causing it to tilt forward. This can strain the lower back. Avoid straight-leg leg-lifts. Instead, while lying on your back, bring your heels up towards your buttocks, and point your knees out (away from each other). You should now be in a"frog-leg" position. Placing your legs in this position removes the hip flexors from the motion and emphasizes the lower abdominal muscles. Put your hands, a pillow, or a towel under your lower back. Now, you can do a modified leg-lift. • Bent-over Rows without support: NEVER do bent-over rows with a barbell. Instead, use a single dumbbell and exercise each side separately. For example, if you are going to exercise your left side, first place your right hand and right knee on a bench (your left foot is on the ground). Now, your spine is supported like a table with 3 legs. • Plank: According to Dr. McGill, a sustained contraction of the long, thin muscles of the back rapidly depletes them of oxygen (McGill SM, et al. 2000). If that is correct, well, that's not good at all! However, as summarized above, he does recommend the side-bridge, but states that it should not be held for longer than 8-10 seconds. • Dead Lifts: If you are looking for 1 exercise with the highest likelihood of producing a back injury, then this is it. People with osteoporosis can injure their back by simply bending over to pick up a pencil. Imagine what kind of pressures are being exerted within your lower spine when you bend over at the waist and try to lift a heavy barbell. SUMMARY The best strategy for dealing with back pain is prevention through regular exercise. But, if you already have back problems, consult your doctor before starting a new routine. Before beginning back-strengthening exercises, keep the following in mind: • Begin slowly. Your back muscles may be weak and susceptible to injury if you're out of shape. Pace yourself. As you get stronger, work up to 15 minutes of exercise a day. • Weight-machines: Use a very light weight and do a high number of repetitions. Pick a weight where you can do at least 20 reps in a row. Your goal is to develop your core muscles by increasing muscular endurance. • Yoga/isometric exercises: Remember not to hold these positions for longer than 5-6 seconds. • Consider hiring a certified personal trainer. Research shows that a custom-designed back-strengthening program achieves better results than when a standardized (ie., "one-size-fits-all") approach is used (Descarreaux M, et al. 2002). If you need medical rehab of your back, then a physical therapist should be consulted. When to See a Doctor About Your Back Pain If you experience any of the following signs, immediately consult with your physician: - Pain that does not go away after two days of rest
- Numbness, weakness, or tingling down the leg to the feet and toes or the inability to move your toes
- Loss of bladder or bowel control
- You feel ill as a result of this episode of back pain
FOR MORE INFORMATION Dr. McGill's review "Core Training: Evidence Translating to Better Performance and Injury Prevention" in the June 2010 issue of the Strength and Conditioning Journal is superb. A highly-regarded book is Dr. McGill's Low Back Disorders: Evidence-Based Prevention and Rehabilitation. Texas Back Institute (TBI) (www.TexasBack.com) is the largest freestanding spine specialty clinic in the US. The Institute, based in Plano, TX, was established in 1977 and provides comprehensive medical care for individuals with back and neck pain. TBI specializes in spinal arthroplasty and minimally invasive spine surgery. TBI's professional staff includes board-certified spine surgeons, internists, chiropractors, physiatrists, pain specialists, exercise physiologists and a team of physical and occupational therapists. As an academic health care organization, TBI has trained hundreds of physicians, scientists and allied health professionals. Its research institution employs state-of-the art technology to treat patients and is actively involved in clinical trials of artificial discs. Readers may be interested in these related stories: MEDICAL TERMINOLOGY Herniated Disc: "Hernia" is a general medical term to describe an organ, or part of an organ, that has pushed through the wall of the cavity where it normally resides. With regards to the spine, a herniated disc describes a disc that has squeezed out of its normal alignment with the vertebrae. This term should not be confused with "subluxation". Sciatica: Sciatic pain is caused by compression of the sciatic nerve, which branches out from the spinal cord at the lumbar and sacral areas. Each of the two branches of this nerve is as wide as a thumb and threads through the pelvis and deep into the buttocks, then down the hip and along the back of the thigh to the foot. Sciatica usually occurs on one side when a sciatic nerve has been stretched or pinched, although spinal stenosis or other vertebral abnormalities can also cause this pain. The sensation of sciatica can vary widely from a mild tingling to severe immobilizing pain. Pain may be experienced in one part of the leg or hip, with numbness in other parts. It typically increases after prolonged standing or sitting and can be aggravated by sudden movements. Spondylolisthesis: Occurs when the lower lumbar vertebra slips forward on the sacrum. Spondylolysis: Literally, the breaking-down of a vertebral structure. Subluxation: A partial, or incomplete, dislocation of a vertebra. EXPERT HEALTH and FITNESS COACHING Stan Reents, PharmD, is available to speak on this and many other exercise-related topics. (Here is a downloadable recording of one of his Health Talks.) He also provides a one-on-one Health Coaching Service. Contact him through the Contact Us page. REFERENCES Altan L, Korkmaz N, Dizdar M, et al. Effect of Pilates training on people with ankylosing spondylitis. Rheumatol Int 2012;32:2093-2099. Abstract Ariyoshi M, Sonoda K, Nagata K, et al. Efficacy of aquatic exercises for patients with low-back pain. Kurume Med J 1999;46:91-96. Abstract Assendelft WJ, Morton SC, Yu EI, et al. Spinal manipulative therapy for low back pain. A meta-analysis of effectiveness relative to other therapies. Ann Intern Med 2003;138:871-881. Abstract Axler C, McGill SM. Low back loads over a variety of abdominal exercises: searching for the safest abdominal challenge. Med Sci Sports Exerc 1997;29:804-811. Abstract Baras T, Baras M, Zeev A, et al. Physical activities and low back pain: a community-based study. Med Sci Sports Exerc 2004;36:9-15. Abstract Brumitt J. Advanced lumbar stabilization exercises. NSCA's Perf Train J 2005;4:11-12. (no abstract) Cox JM, Trier KK. Exercise and smoking habits in patients with and without low back and leg pain. J Manipulative Physiol Ther 1987;10:239-245. Abstract Danneels LA, Vanderstraeten GG, Cambier DC, et al. Effects of three different training modalities on the cross sectional area of the lumbar multifidus muscle in patients with chronic low back pain. Br J Sports Med 2001;35:186-191. Abstract Descarreaux M, Normand MC, Laurencelle L, et al. Evaluation of a specific home exercise program for low back pain. J Manipulative Physiol Ther 2002;25:497-503. Abstract Dundar U, Solak O, Yigit I, et al. Clinical effectiveness of aquatic exercise to treat chronic low back pain: a randomized controlled trial. Spine 2009;34:1436-1440. Abstract Hadler NM, Tait RC, Chibnall JT. Back pain in the workplace. JAMA 2007;297:1594-1596. (no abstract) Harreby M, Hesselsoe G, Kjer J, et al. Low back pain and physical exercise in leisure time in 38-year-old men and women: a 25-year prospective cohort study of 640 school children. Eur Spine J 1997;6:181-186. Abstract Harris CD, Watson KB, Carlson SA, et al. Adult participation in aerobic and muscle-strengthening physical activities: United States, 2011. MMWR 2013;62:326-330. Hodges PW, Richardson CA. Inefficient muscular stabilization of the lumbar spine associated with low back pain. Spine 1996;21:2640-2650. Abstract Lee BCY, McGill SM. Effect of long-term isometric training on core/torso stiffness. J Strength Cond Res 2015;29:1515-1526. Abstract Mannion AF, Muntener M, Taimela S, et al. A randomized clinical trial of three active therapies for chronic low back pain. Spine 1999;24:2435-2448. Abstract Mannion AF, Muntener M, Taimela S, et al. Comparison of three active therapies for chronic low back pain: results of a randomized clinical trial with one-year follow-up. Rheumatology 2001;40:772-778. Abstract Marshall PW, Kennedy S, Brooks C, et al. Pilates exercise or stationary cycling for chronic non-specific low back pain: Does it matter? A randomized controlled trial with 6-month follow-up. Spine 2013;38:E952-E959. Abstract McGill SM, Hughson RL, Parks K. Lumbar erector spinae oxygenation during prolonged contractions. Ergonomics 2000;43:486-493. Abstract McGill SM. Low back stability: From formal description to issues for performance and rehabilitation. Exercise Sport Sci Rev 2001;29:26-31. Abstract McGill S. Core training: Evidence translating to better performance and injury prevention. Strength Conditioning J 2010;32:33-46. Link Mundt DJ, Kelsey JL, Golden AL, et al. An epidemiologic study of sports and weight lifting as possible risk factors for herniated lumbar and cervical discs. Am J Sports Med 1993;21:854-860. Abstract Nyska M, Constantini N, Cale-Benzoor M, et al. Spondylolysis as a cause of low back pain in swimmers. Int J Sports Med 2000;21:375-379. Abstract Ong A, Anderson J, Roche J. A pilot study of the prevalence of lumbar disc degeneration in elite athletes with lower back pain at the Sydney 2000 Olympic Games. Br J Sports Med 2003;37:263-266. Abstract Rasmussen-Barr E, Nilsson-Wikmar L, Arvidsson I. Stabilizing training compared with manual treatment in sub-acute and chronic low-back pain. Manual Therapy 2003;8:233-241. Abstract Standaert CJ, Friedly J, Erwin MW, et al. Comparative effectiveness of exercise, acupuncture, and spinal manipulation for low back pain. Spine 2011;36:S120-S130. Abstract Torstensen TA, Ljunggren AE, Meen HD, et al. Efficiency and costs of medical exercise therapy, conventional physiotherapy, and self-exercise in patients with chronic low back pain: A pragmatic, randomized, single-blinded, controlled trial with 1-year follow-up. Spine 1998;23:2616-2624. Abstract Volinn E. The epidemiology of low-back pain in the rest of the world. Spine 1997;22:1747-1754. Abstract Waller B, Lambeck J, Daly D. Therapeutic aquatic exercise in the treatment of low back pain: A systematic review. Clin Rehabil 2009;23:3-14. Abstract ABOUT THE AUTHOR 
Stan Reents, PharmD, is a former healthcare professional. He has been a member of the American College of Lifestyle Medicine (ACLM) and a member of the American College of Sports Medicine (ACSM). In the past, he has been certified as a Health Fitness Specialist by ACSM, as a Certified Health Coach by ACE, as a Personal Trainer by ACE, and as a tennis coach by USTA. He is the author of Sport and Exercise Pharmacology (published by Human Kinetics) and has written for Runner's World magazine, Senior Softball USA, Training and Conditioning and other fitness publications.
Browse By Topic:
back pain, exercise and health, exercise guidelines, exercise recommendations, health and fitness targets, osteoporosis, sports medicine
Copyright ©2026 AthleteInMe,
LLC. All rights reserved.
|